People may comment that an individual seems to have “sensory issues” but what does this mean?
“Sensory” refers to the senses: hearing, sight, smell, touch, taste, body awareness, movement, and balance. Sensations are brain-based functions, in other words, the brain controls what and how we perceive sensations.
How does the brain process the senses?
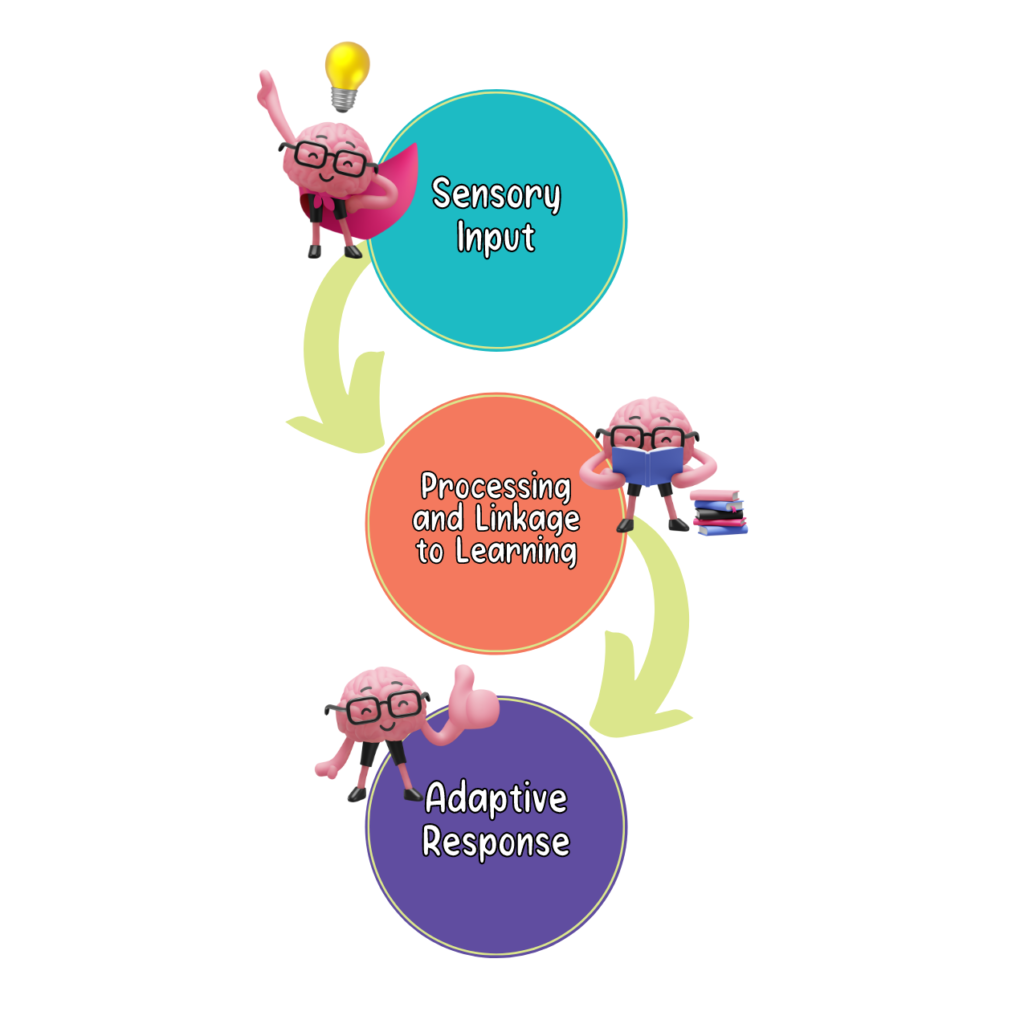
The healthy brain takes in sensory information from the environment (‘sensory input’) through our eyes, ears, nose, mouth, and skin. This information is then processed rapidly in the brain and connected to previously learned experiences. The individual then responds or reacts to the sensory input in a manner that keeps the individual safe, healthy, and alive; this is called an “adaptive response.”
Individuals with neurodevelopmental or mental health diagnoses such as Autism Spectrum Disorder, Attention-Deficit-Hyperactivity-Disorder, or Tourette’s Syndrome have differences in brain wiring when compared to typical individuals. This means that the way in which the brain receives, processes, and responds to sensory input may be different than expected. For example, an individual with sensory hypersensitivities may become agitated and upset in a loud, busy shopping mall or complain of a shirt with a sewn-in logo feeling ‘scratchy’ or uncomfortable.
Sensory Preferences
We can all have sensory preferences without having a sensory processing disorder.
This means that some of us enjoy jumping out of bed in the morning, opening the blinds to feel the sunshine, playing loud music, or going for a jog. Others prefer to start the morning out slowly, with minimal noise until their brain feels ‘awake’ enough to tolerate more stimulation. Some individuals love spicy food, scented lotions, or wild rides at the Red River Ex and others prefer to stay at home quietly reading a book.
Sensory preferences can change from day-to-day or hour-to-hour. We may enjoy a hot cup of coffee one day and prefer a cold iced latte the next. Our preferences change depending on many factors including amount of sleep we have had, whether we are stressed about something, if we are ill, if we have body pain, or if we feel calm and ready to engage in our day.
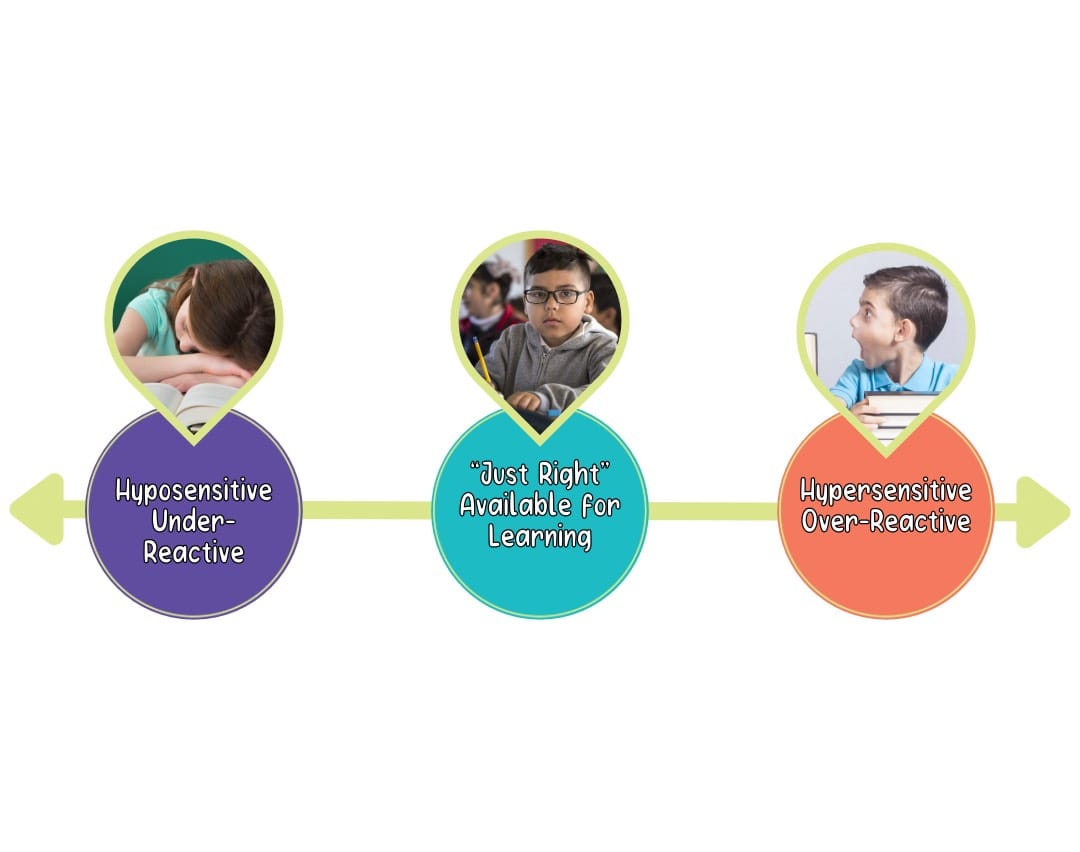
Sensory Processing Continuum
The goal is to support the child’s ability to remain in the middle of the continuum so that the child’s brain is at a “just right” level of physiological arousal and is, therefore, in a state that is most conducive to learning.
Individuals with altered sensory processing also have preferences and these too can change from moment to moment. This means that certain strategies that are effective one day may not be as effective the next. Supporting individuals with sensory issues means paying close attention to cues to over- and under- stimulation.
Becoming a Detective

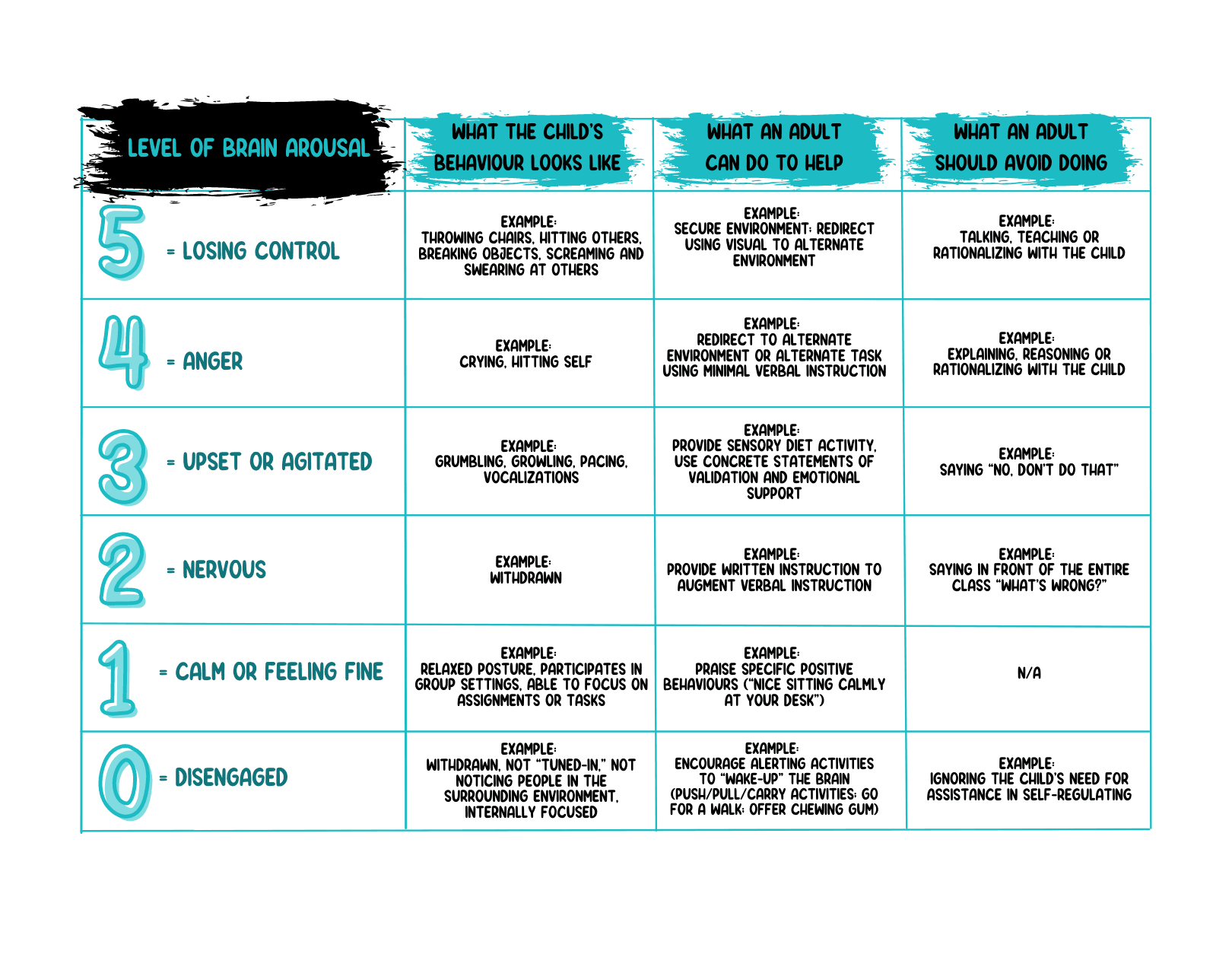
Adults supporting individuals with altered sensory processing are encouraged to be “detectives” by paying close attention to the individual’s cues to under- and over-stimulation.
Many children are not aware of their own needs for sensory-regulating activities. It requires the assistance of supporting adults to prompt a child to access tools for self-regulation. Each child will display their own unique mannerisms or cues that can indicate either a need for increased sensory stimulation or that sensory overload is fast-approaching. Some examples of cues to look for are humming, tapping surfaces, spinning in circles, vocalizing repetitive sounds, pacing, rocking, appearing withdrawn or “shutting down” or becoming self-injurious. Tracking a child’s individual behaviors (cues) is useful information. These cues can then be shared with the adults in the child’s support network (at home, school, daycare and in the community) so that everyone is aware of what to watch for and how to respond to specific cues consistently across environments.

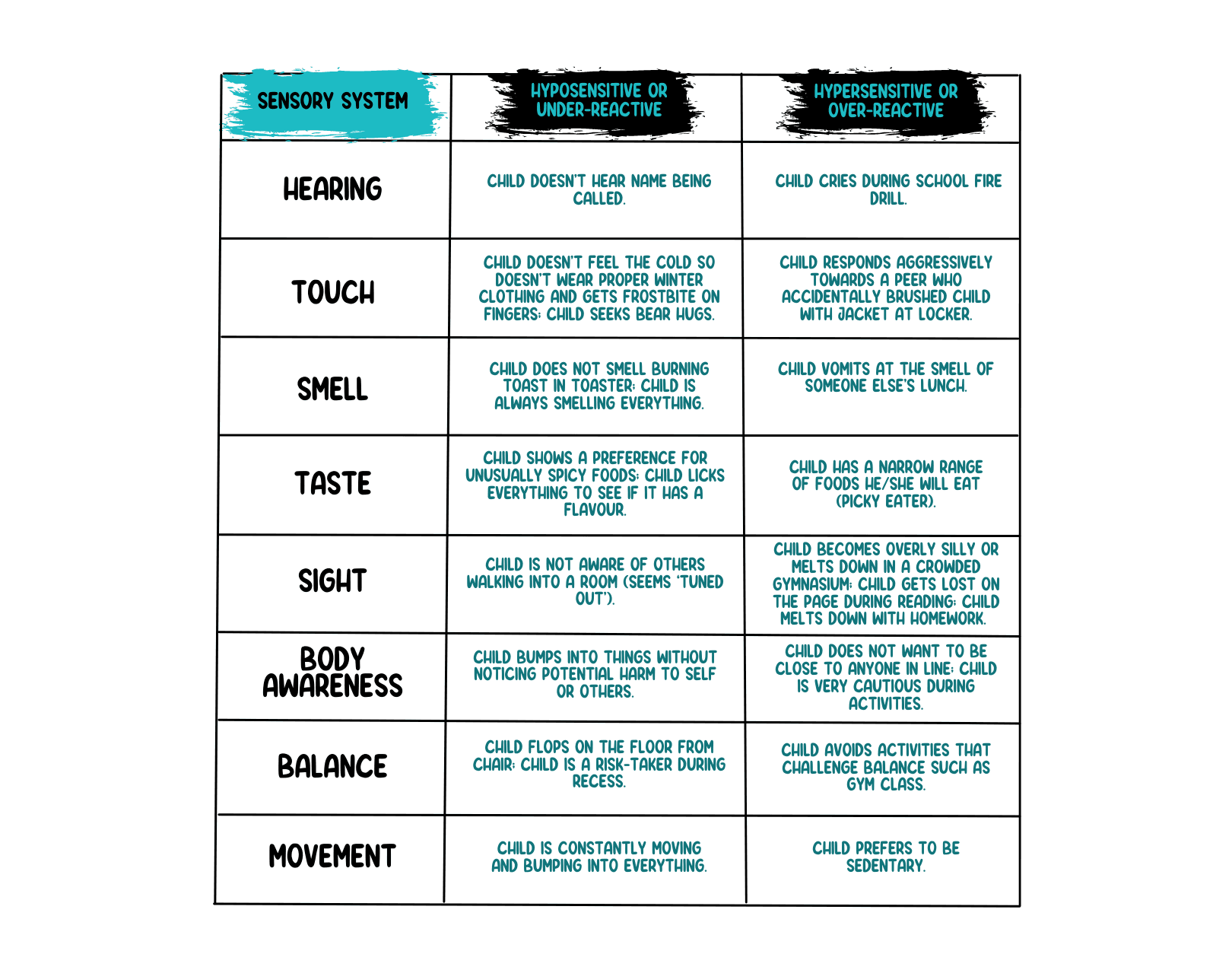
Examples of Difficulties in Daily Functioning Related to Sensory Processing

If you suspect that someone has a sensory processing disorder, please ask an occupational therapist to conduct a sensory processing assessment. Formal testing can be done to determine an individual’s sensory needs and improve that individual’s ability to cope with the demands of daily living at home, school, or in the community.
Thank you,
Tamara Rogers, MSc., BMR (OT), OT Reg. (MB)
Outreach Clinician

MORE COMMON THAN YOU THINK
- 1 in 7 children suffers from mental illness in Manitoba (Chartier et al., 2016).
- 70% of mental health problems have their onset in childhood or adolescence (Government of Canada, 2006).
There Is Hope The good news is that mental illness can be treated effectively. There are things that can be done to prevent mental illness and its impact and help improve the lives of children experiencing mental health concerns. Early intervention is best.
How KIDTHINK Can Help
To make a referral contact us
To subscribe to our newsletter, click the 'subscribe' button.




